Ultrasound: pelvic: Difference between revisions
(Created page with "*Definite IUP = gestational sac containing yolk sac **Occurs ~5th week ==See Also== Ultrasound (Main) ==Source== Sonoguide Category:Rads Category:OB/GYN") |
m (Danbot moved page Ultrasound: Pelvic to Ultrasound: pelvic without leaving a redirect: Naming convention: first word capitalized, subsequent words lowercase) |
||
| (36 intermediate revisions by 8 users not shown) | |||
| Line 1: | Line 1: | ||
* | ''See [[pelvic ultrasound (transabdominal)]] and [[pelvic ultrasound (transvaginal)]] for more detailed info on technique and findings'' | ||
** | ==Background== | ||
[[File:Pregnancy timeline.png|thumb|Timeline of pregnancy, including (from top to bottom): Trimesters, embryo/fetus development, gestational age in weeks and months, viability and maturity stages.]] | |||
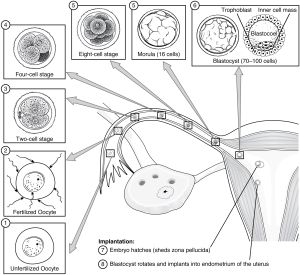
[[File:2904 Preembryonic Development-02.jpg|thumb|Pre-embryonic development.]] | |||
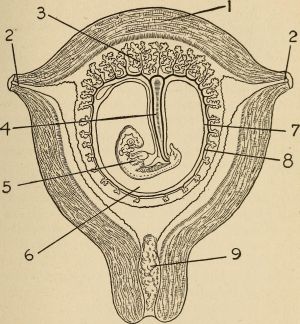
[[File:Maternity and child care (1920) (14593999138).jpg|thumb|Cross section of pregnant uterus (second month of gestation): 1—Wall of uterus. 2—Beginning of fal-lopian tube. 3—Placenta showing branches of villi.4—Umbilical cord. 5—Fetus. 6—Amnionicfluid or bag of waters. 7—Amnionicmembrane. 8—Chorionic membrance.9—Cervix or mouth of uterus.]] | |||
*Ultrasound is the preferred imaging modality for the female pelvic organs | |||
==Indications== | |||
*To evaluate female reproductive organs in pediatric patients or those that are not sexually active or refuse transvaginal exam | |||
*Start with transabdominal ultrasound when evaluating to rule out ectopic (less invasive than transvaginal), particularly if bHCG >6,000 | |||
===General=== | |||
*[[Pelvic pain]] | |||
*Abnormal pelvic or abdominal exam | |||
===Uterus=== | |||
*[[Vaginal bleeding]] | |||
*Fibroids | |||
*IUD placement | |||
===Ovaries and adnexa=== | |||
*[[Ovarian cyst]] | |||
*[[Ovarian torsion]] | |||
*Ovarian masses | |||
*[[Tubo-ovarian abscess]] | |||
*Hydrosalpinx | |||
===[[Pregnancy]]=== | |||
*Confirm intrauterine pregnancy | |||
*Gestational dating | |||
*Fetal monitoring and surveillance | |||
*Evaluation of placenta | |||
*[[Spontaneous abortion]] | |||
*[[Intrauterine fetal demise]] | |||
*[[Ectopic pregnancy]] | |||
*Heterotopic pregnancy | |||
*[[Molar pregnancy]] | |||
==Technique== | |||
===[[pelvic ultrasound (transabdominal)|Transabdominal]]=== | |||
*3.5 MHz curvilinear probe | |||
*Start above pubic symphysis in longitudinal axis | |||
*Locate endometrial stripe (echogenic line) which represents the center of the uterus | |||
*Scan through longitudinal axis of uterus and sweep laterally to try to visualize ovaries (though often difficult to visualize on transabdominal ultrasound) | |||
*Rotate probe to transverse plane above pubic symphysis and scan through uterus from cervix to fundus | |||
*Scan hepatorenal recess to assess for free fluid | |||
===[[pelvic ultrasound (transvaginal)|Transvaginal]]=== | |||
====General==== | |||
*Use 5 MHz endocavitary probe (high frequency, low penetration) | |||
*Apply surgical lubricant inside and outside probe cover | |||
*Place patient in lithotomy position | |||
*Gently advance probe into vaginal canal and position adjacent to cervix | |||
**May be more comfortable for patient to insert probe into vagina herself | |||
*Apply gentle pressure to lower abdominal wall with one hand and manipulate probe with other hand | |||
====Longitudinal scan==== | |||
*Probe marker pointing at 12:00 | |||
*Shows anterior structures on left side of screen | |||
*Begin midline at endometrial stripe | |||
*Scan from right to left through uterus | |||
*Move probe laterally to view adnexa and ovaries | |||
====Transverse scan==== | |||
*Rotate probe 90 degrees counterclockwise so probe marker is pointing at 9:00 | |||
*Shows right-sided structures on left side of screen | |||
*Start at endometrial stripe and scan throughout uterus | |||
*Locate cornual flare (junction of uterus and fallopian tubes) | |||
*Move probe laterally along fallopian tube to locate ovary | |||
*Ovaries identified by follicular (anechoic or hypoechoic) structures | |||
<gallery mode="packed"> | |||
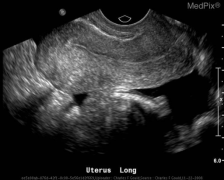
File:longitudinal uterus.jpg|Uterus in longitudinal plane | |||
File:cornual flare.jpg|Cornual flare (uterus and fallopian tube junction) in transverse plane | |||
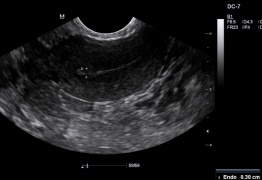
File:ovary with follicles.jpg|Normal ovary with follicles | |||
</gallery> | |||
==Normal Findings== | |||
===Uterus=== | |||
*Anteverted: Fundus pointing to anterior abdominal wall | |||
*Retroverted: Fundus pointing to posterior wall | |||
*Endometrial stripe: Measured from thickest echogenic area (from one basal endometrial interface to the other, including canal) | |||
**Pre-menopausal: | |||
***During menstruation: 2-4mm | |||
***Early proliferative phase: 5-7mm | |||
***Late proliferative phase: 11mm | |||
***Secretory phase: 7-16mm | |||
***After D&C or SAB: >5mm | |||
****Consider retained POC if thicker | |||
**Post-menopausal: | |||
***With vaginal bleeding: <5mm | |||
***Without vaginal bleeding: <11mm | |||
<gallery mode="packed"> | |||
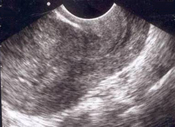
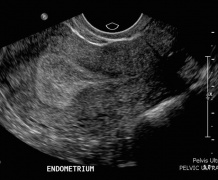
File:secretory_endometrium.jpg|Normal thickened endometrial stripe during secretory phase | |||
File:Menstrual_endometrium.JPG|Normal thin endometrial stripe during menses | |||
</gallery> | |||
===Ovaries=== | |||
*Physiologic cysts present | |||
**<3 cm diameter | |||
**Ovarian follicle or corpus luteum | |||
**Typically don't cause complications | |||
===[[Pregnancy]] (1st trimester)=== | |||
*4-5 weeks | |||
**Gestational sac | |||
***First sign of early pregnancy, usually seen between 3-5 weeks gestation | |||
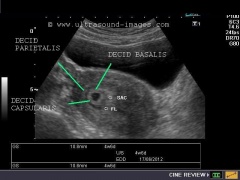
**"Double decidual sac" sign | |||
***Two concentric rings (uterine lining and gestation lining) around anechoic gestational sac) | |||
***Highly suggestive of intrauterine pregnancy (before yolk sac or embryo embryo visualized | |||
**"Intradecidual sign" | |||
***Thickened decidua on one side of uterine cavity surrounding anechoeic sac | |||
*5-6 weeks: | |||
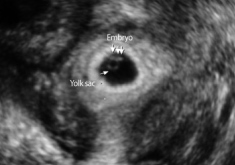
**Yolk Sac | |||
***Circular (or sometimes as two parallel lines) echogenic structure with thick walls within gestational sac | |||
***Definitive evidence of intrauterine pregnancy | |||
***Multiple yolk sacs is earliest sign in multiple gestational pregnancy | |||
**"Double bleb" sign | |||
***Yolk sac and amniotic cavity that look like two bubbles within gestational sac | |||
*6-7 weeks | |||
**Fetal Pole | |||
***First visual manifestation of fetus (or "embryo") | |||
***Thickening of margin on yolk sac | |||
**Cardiac activity present (FHR ~100-115 bpm) | |||
**Crown rump length: ~5mm | |||
*8-9 weeks | |||
**Limb buds appear | |||
**Head identifiable | |||
*9-10 weeks | |||
**FHR ~170-180 bpm | |||
**Fetal movement visible | |||
**End of embryonic period | |||
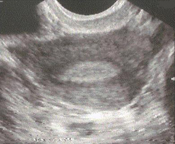
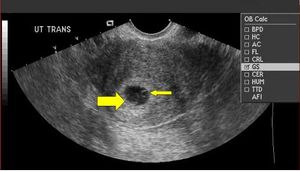
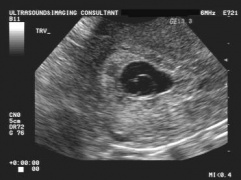
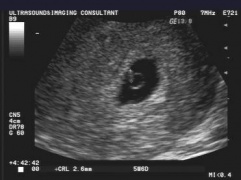
[[File:yolk sac.jpg|thumbnail|In a normal pregnancy, the gestational sac appears as a hypoechoic structure encircled by an echogenic border within the endometrial cavity at 4-5 weeks]] | |||
[[File:IUP.jpg|thumb|IUP at 6 wks]] | |||
<gallery mode="packed"> | |||
File:double_decidual_sac_sign.jpg|Double decidual sac sign | |||
File:intradecidual sign.jpg|Intradecidual sign | |||
File:double_bleb_sign.jpg|Double bleb sign (yolk sac and amniotic cavity) | |||
File:fetal_pole.jpg|Fetal pole (Thickening of yolk sac on one side) | |||
</gallery> | |||
==Abnormal Findings== | |||
===Abnormal Pregnancy=== | |||
*Gestational sac >10mm without visible yolk sac | |||
*Gestational sac >18mm without fetal pole | |||
*Collapsed gestational sac | |||
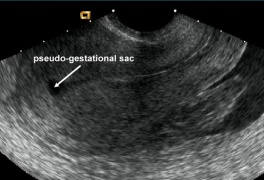
*Pseudogestational sac | |||
**Endometrial breakdown during [[ectopic pregnancy]] | |||
**May be erroneously interpreted as true gestational sac in ectopic pregnancy | |||
**Irregularly shaped | |||
**Located in endometrial cavity, instead of eccentrically within endometrium | |||
**No yolk sac present | |||
**May not have double decidual sac sign | |||
*Absence of fetal heart beat in embryo with CRL >5mm | |||
*FHR <90 bpm | |||
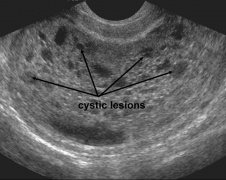
*[[Molar pregnancy]] | |||
**Many small, irregular cystic structures in endometrium | |||
**"Snowstorm appearance" | |||
<gallery mode="packed"> | |||
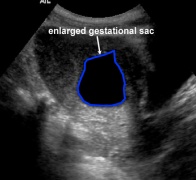
File:large gestational sac.jpg|Gestational sac greater than 10mm without yolk sac | |||
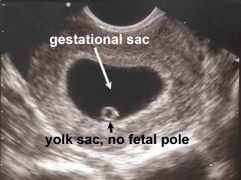
File:Gestational_sac_without_fetal_pole.jpg|Gestational sac greater than 18mm without fetal pole | |||
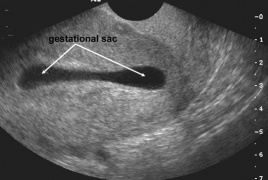
File:collapsed gestational sac.jpg|Collapsed gestational sac | |||
File:pseudogestational sac.jpg|Pseudogestational sac | |||
File:molar pregnancy.jpg|Molar pregnancy with multiple cystic lesions in endometrium ("snowstorm appearance") | |||
</gallery> | |||
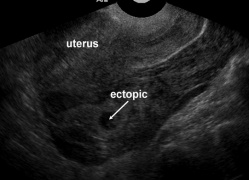
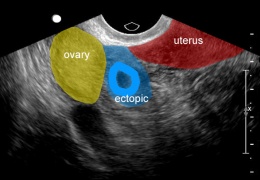
====[[Ectopic pregnancy]]==== | |||
*Implantation of blastocyst outside of endometrium | |||
*Occur in fallopian tubes, cervix, ovaries, peritoneal cavity, or scar of prior uterine surgery | |||
*Most definitive sonographic sign is gestational sac with yolk sac, embryo, or fetal heart beat outside of the endometrium | |||
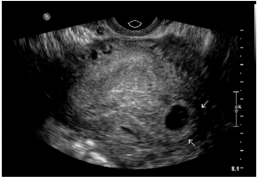
*Tubal pregnancy | |||
**"Tubal ring" sign: echogenic thick-walled anechoic sac visualized between uterus and ovary (separate from ovary when pressure applied to fallopian tube with probe) | |||
*Interstitial Pregnancy | |||
**Implantation of gestational sac in muscular wall of uterus at proximal regional of fallopian tubes | |||
**"Interstitial line" sign: hyperechoic line from endometrial stripe to cornual region adjacent to interstitial gestational sac | |||
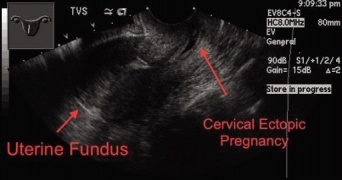
*Cervical Pregnancy | |||
**Implantation of gestational sac below internal cervical os | |||
**Can cause life-threatening hemorrhage | |||
**Must distinguish between cervical ectopic and spontaneous abortion at level of cervix: | |||
{| {{table}} | |||
| align="center" style="background:#f0f0f0;"|'''Cervical ectopic''' | |||
| align="center" style="background:#f0f0f0;"|'''Spontaneous abortion at cervix''' | |||
|- | |||
| Hour-glass shaped uterus||Elongated gestational sac | |||
|- | |||
| Gestational sac with yolk sac, fetal pole, or heartbeat||Absent embryonic cardiac activity | |||
|- | |||
| Closed internal os||Dilated internal os | |||
|- | |||
| Color doppler showing hypervascular trophoblastic ring||Sac moves in cervix with gentle probing (“Sliding sac sign”) | |||
|- | |||
| Empty uterine cavity||Loss of sac on serial imaging | |||
|- | |||
| | |||
|} | |||
<gallery mode="packed"> | |||
File:ectopic pregnancy.jpg|Ectopic pregnancy | |||
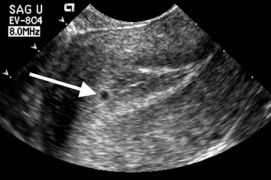
File:free_fluid_ectopic.png|Free fluid in cul-de-sac with no gestational sac visualized in uterus | |||
File:tubal ring.jpg|Ectopic pregnancy between ovary and uterus, suggestive of tubal ectopic | |||
File:interstitial pregnancy.png|Interstitial pregnancy | |||
File:cervical ectopic.jpg|Cervical pregnancy | |||
</gallery> | |||
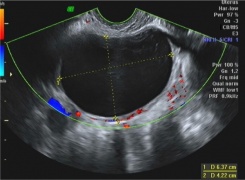
===[[Ovarian Torsion]]=== | |||
*Bimodal age distribution: young women (15-30yo) and post-menopausal women | |||
*Typically occur in enlarged ovaries (>5cm) | |||
**Benign mature cystic teratomas | |||
**Hemorrhagic/large ovarian cysts | |||
**Cystic neoplasms | |||
**Cystadenomas | |||
**Polycystic ovarian syndrome | |||
*Sonographic signs associated with torsion | |||
**Enlarged ovary from edema, engorgement, hemorrhage | |||
**Midline ovary | |||
**Free pelvic fluid | |||
**Underlying ovarian lesions | |||
**Peripherally displaced follicular cysts | |||
**Doppler findings: | |||
***Decreased/absent venous or arterial flow | |||
***Absent/reversed diastolic flow | |||
***Can have normal flow (from dual supply from uterine and ovarian arteries) | |||
<gallery mode="packed"> | |||
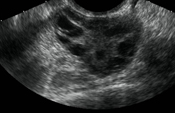
File:simple_cyst.jpg|Large ovarian cystadenoma | |||
File:hemorrhagic_cyst.jpg|Hemorrhagic ovarian cyst with blood clot | |||
File: ovarian_torsion 1.png|Large midline ovary with multiple peripherally located follicular cysts (torsion) | |||
File:absent_waveforms.png|Absent color doppler and venous and arterial waveforms (torsion) | |||
</gallery> | |||
==Pearls and Pitfalls== | |||
*Free pelvic fluid with positive hCG is ectopic pregnancy until proven otherwise | |||
*Presence of doppler flow cannot rule out ovarian torsion | |||
==See Also== | ==See Also== | ||
== | *[[Ultrasound (Main)]] | ||
*[[Pelvic ultrasound (transabdominal)]] | |||
*[[Pelvic ultrasound (transvaginal)]] | |||
*[[Ectopic Pregnancy]] | |||
==References== | |||
<references/> | |||
[[Category: | [[Category:Radiology]] [[Category:OBGYN]] | ||
[[Category: | [[Category:Ultrasound]] | ||
Latest revision as of 05:35, 22 March 2026
See pelvic ultrasound (transabdominal) and pelvic ultrasound (transvaginal) for more detailed info on technique and findings
Background
- Ultrasound is the preferred imaging modality for the female pelvic organs
Indications
- To evaluate female reproductive organs in pediatric patients or those that are not sexually active or refuse transvaginal exam
- Start with transabdominal ultrasound when evaluating to rule out ectopic (less invasive than transvaginal), particularly if bHCG >6,000
General
- Pelvic pain
- Abnormal pelvic or abdominal exam
Uterus
- Vaginal bleeding
- Fibroids
- IUD placement
Ovaries and adnexa
- Ovarian cyst
- Ovarian torsion
- Ovarian masses
- Tubo-ovarian abscess
- Hydrosalpinx
Pregnancy
- Confirm intrauterine pregnancy
- Gestational dating
- Fetal monitoring and surveillance
- Evaluation of placenta
- Spontaneous abortion
- Intrauterine fetal demise
- Ectopic pregnancy
- Heterotopic pregnancy
- Molar pregnancy
Technique
Transabdominal
- 3.5 MHz curvilinear probe
- Start above pubic symphysis in longitudinal axis
- Locate endometrial stripe (echogenic line) which represents the center of the uterus
- Scan through longitudinal axis of uterus and sweep laterally to try to visualize ovaries (though often difficult to visualize on transabdominal ultrasound)
- Rotate probe to transverse plane above pubic symphysis and scan through uterus from cervix to fundus
- Scan hepatorenal recess to assess for free fluid
Transvaginal
General
- Use 5 MHz endocavitary probe (high frequency, low penetration)
- Apply surgical lubricant inside and outside probe cover
- Place patient in lithotomy position
- Gently advance probe into vaginal canal and position adjacent to cervix
- May be more comfortable for patient to insert probe into vagina herself
- Apply gentle pressure to lower abdominal wall with one hand and manipulate probe with other hand
Longitudinal scan
- Probe marker pointing at 12:00
- Shows anterior structures on left side of screen
- Begin midline at endometrial stripe
- Scan from right to left through uterus
- Move probe laterally to view adnexa and ovaries
Transverse scan
- Rotate probe 90 degrees counterclockwise so probe marker is pointing at 9:00
- Shows right-sided structures on left side of screen
- Start at endometrial stripe and scan throughout uterus
- Locate cornual flare (junction of uterus and fallopian tubes)
- Move probe laterally along fallopian tube to locate ovary
- Ovaries identified by follicular (anechoic or hypoechoic) structures
Normal Findings
Uterus
- Anteverted: Fundus pointing to anterior abdominal wall
- Retroverted: Fundus pointing to posterior wall
- Endometrial stripe: Measured from thickest echogenic area (from one basal endometrial interface to the other, including canal)
- Pre-menopausal:
- During menstruation: 2-4mm
- Early proliferative phase: 5-7mm
- Late proliferative phase: 11mm
- Secretory phase: 7-16mm
- After D&C or SAB: >5mm
- Consider retained POC if thicker
- Post-menopausal:
- With vaginal bleeding: <5mm
- Without vaginal bleeding: <11mm
- Pre-menopausal:
Ovaries
- Physiologic cysts present
- <3 cm diameter
- Ovarian follicle or corpus luteum
- Typically don't cause complications
Pregnancy (1st trimester)
- 4-5 weeks
- Gestational sac
- First sign of early pregnancy, usually seen between 3-5 weeks gestation
- "Double decidual sac" sign
- Two concentric rings (uterine lining and gestation lining) around anechoic gestational sac)
- Highly suggestive of intrauterine pregnancy (before yolk sac or embryo embryo visualized
- "Intradecidual sign"
- Thickened decidua on one side of uterine cavity surrounding anechoeic sac
- Gestational sac
- 5-6 weeks:
- Yolk Sac
- Circular (or sometimes as two parallel lines) echogenic structure with thick walls within gestational sac
- Definitive evidence of intrauterine pregnancy
- Multiple yolk sacs is earliest sign in multiple gestational pregnancy
- "Double bleb" sign
- Yolk sac and amniotic cavity that look like two bubbles within gestational sac
- Yolk Sac
- 6-7 weeks
- Fetal Pole
- First visual manifestation of fetus (or "embryo")
- Thickening of margin on yolk sac
- Cardiac activity present (FHR ~100-115 bpm)
- Crown rump length: ~5mm
- Fetal Pole
- 8-9 weeks
- Limb buds appear
- Head identifiable
- 9-10 weeks
- FHR ~170-180 bpm
- Fetal movement visible
- End of embryonic period
Abnormal Findings
Abnormal Pregnancy
- Gestational sac >10mm without visible yolk sac
- Gestational sac >18mm without fetal pole
- Collapsed gestational sac
- Pseudogestational sac
- Endometrial breakdown during ectopic pregnancy
- May be erroneously interpreted as true gestational sac in ectopic pregnancy
- Irregularly shaped
- Located in endometrial cavity, instead of eccentrically within endometrium
- No yolk sac present
- May not have double decidual sac sign
- Absence of fetal heart beat in embryo with CRL >5mm
- FHR <90 bpm
- Molar pregnancy
- Many small, irregular cystic structures in endometrium
- "Snowstorm appearance"
Ectopic pregnancy
- Implantation of blastocyst outside of endometrium
- Occur in fallopian tubes, cervix, ovaries, peritoneal cavity, or scar of prior uterine surgery
- Most definitive sonographic sign is gestational sac with yolk sac, embryo, or fetal heart beat outside of the endometrium
- Tubal pregnancy
- "Tubal ring" sign: echogenic thick-walled anechoic sac visualized between uterus and ovary (separate from ovary when pressure applied to fallopian tube with probe)
- Interstitial Pregnancy
- Implantation of gestational sac in muscular wall of uterus at proximal regional of fallopian tubes
- "Interstitial line" sign: hyperechoic line from endometrial stripe to cornual region adjacent to interstitial gestational sac
- Cervical Pregnancy
- Implantation of gestational sac below internal cervical os
- Can cause life-threatening hemorrhage
- Must distinguish between cervical ectopic and spontaneous abortion at level of cervix:
| Cervical ectopic | Spontaneous abortion at cervix |
| Hour-glass shaped uterus | Elongated gestational sac |
| Gestational sac with yolk sac, fetal pole, or heartbeat | Absent embryonic cardiac activity |
| Closed internal os | Dilated internal os |
| Color doppler showing hypervascular trophoblastic ring | Sac moves in cervix with gentle probing (“Sliding sac sign”) |
| Empty uterine cavity | Loss of sac on serial imaging |
Ovarian Torsion
- Bimodal age distribution: young women (15-30yo) and post-menopausal women
- Typically occur in enlarged ovaries (>5cm)
- Benign mature cystic teratomas
- Hemorrhagic/large ovarian cysts
- Cystic neoplasms
- Cystadenomas
- Polycystic ovarian syndrome
- Sonographic signs associated with torsion
- Enlarged ovary from edema, engorgement, hemorrhage
- Midline ovary
- Free pelvic fluid
- Underlying ovarian lesions
- Peripherally displaced follicular cysts
- Doppler findings:
- Decreased/absent venous or arterial flow
- Absent/reversed diastolic flow
- Can have normal flow (from dual supply from uterine and ovarian arteries)
Pearls and Pitfalls
- Free pelvic fluid with positive hCG is ectopic pregnancy until proven otherwise
- Presence of doppler flow cannot rule out ovarian torsion
See Also
- Ultrasound (Main)
- Pelvic ultrasound (transabdominal)
- Pelvic ultrasound (transvaginal)
- Ectopic Pregnancy